Fixing IT band syndrome (the inflammation and pain along the iliotibial band on the outer side of the thigh, typically presenting as lateral knee pain or lateral hip pain that worsens with activities like running, cycling, and prolonged knee flexion – typically caused by a combination of weak hip stabilizers and IT band tightness) requires understanding both the contributing factors (most IT band syndrome develops from a combination of: 1) weak gluteus medius – the primary contributor to IT band syndrome, with weak hip stabilizers producing the hip mechanics that overload the IT band, 2) tight IT band and lateral hip muscles, 3) weak gluteal complex contributing to overall hip dysfunction, 4) training errors like rapid mileage increases or overtraining in runners, 5) limited hip mobility, 6) muscle imbalances between hip stabilizers and prime movers, 7) inadequate cross-training, or 8) the cumulative effect of multiple factors) and the training principles that resolve them: gluteus medius strengthening as the primary intervention (clamshells, side hip abductions) – the single most important intervention for IT band syndrome, IT band stretching (standing iliotibial stretch) for direct lateral hip flexibility, deep glute and hip rotator stretching for the entire hip complex, compound glute strengthening (glute bridges) for overall hip strength, lateral core stability (side plank), unilateral hip mechanics training (step-ups, single-leg deadlifts) for functional integration, and thoracic mobility for integrated movement. Most non-severe cases of IT band syndrome improve substantially within 6 to 12 weeks of consistent intervention. Note: severe or persistent cases warrant medical evaluation. Some general health information is provided here, but individual circumstances vary – consulting a qualified healthcare provider or physical therapist is recommended for severe pain or persistent symptoms.
Below are ten of the most effective exercises for fixing IT band syndrome, covering primary IT band stretching (standing iliotibial stretch), deep hip flexibility (seated piriformis stretch), gluteus medius strengthening (side-lying clam, side hip abduction), compound glute strengthening (barbell glute bridge), lateral core stability (side plank), thoracic mobility integration (foam roll serratus wall slide), unilateral hip mechanics (dumbbell step-up, bodyweight single-leg deadlift), and thoracic mobility (open book stretch). Together they form a comprehensive IT band syndrome correction program. A 20 to 30-minute session pulled from this list, performed 4 to 6 times per week (daily during initial correction phase), produces measurable improvement within 6 to 12 weeks of consistent practice for most non-severe cases. Combine gluteus medius strengthening with IT band stretching for maximum effectiveness – strengthening alone or stretching alone produces slower results than combined intervention.
Standing Iliotibial Stretch
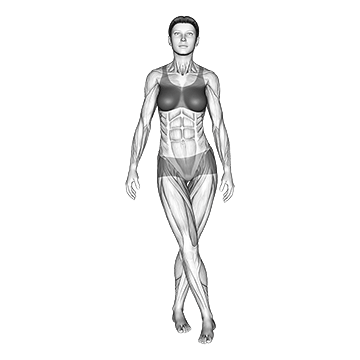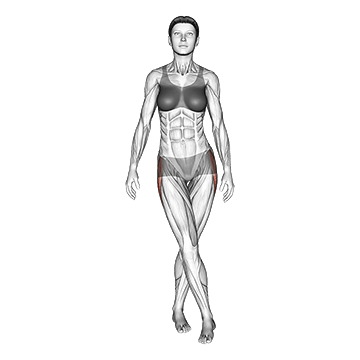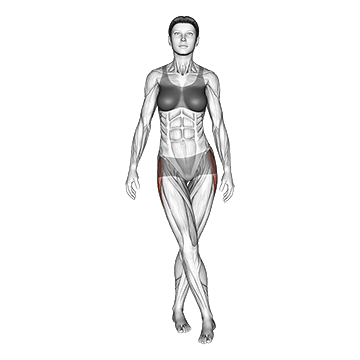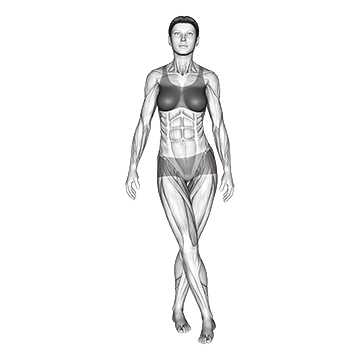
The Standing Iliotibial Stretch performs IT band stretching. The pattern is foundational for IT band syndrome correction.
For IT band syndrome correction, the standing iliotibial stretch is foundational. Run it for 3 sets of 30 to 60-second holds per side, multiple times daily.
Stand tall with feet hip-width. Cross one leg behind the other. Lean toward the side of the back leg, bringing the arm of the back leg overhead toward the opposite side. Feel deep stretch through the side of the hip and down the IT band of the back leg. Hold for 30 to 60 seconds. Switch sides. The pattern is foundational for IT band syndrome correction – daily multi-session IT band stretching addresses the lateral hip and IT band tightness contributing to the condition. The stretch can be done anywhere with minimal equipment, supporting the high frequency that IT band correction responds to.
Seated Piriformis Stretch

The Seated Piriformis Stretch performs piriformis stretching. The pattern addresses deep glute and hip flexibility.
For IT band syndrome correction, the seated piriformis stretch addresses related deep hip flexibility. Run it for 3 sets of 30 to 60-second holds per side, daily.
Sit on the floor with one leg extended and the other leg crossed over with the foot planted on the floor on the opposite side. Pull the knee of the crossed leg toward the opposite shoulder while rotating the torso. Feel deep stretch in the glute. Hold for 30 to 60 seconds. Switch sides. The pattern produces direct piriformis and deep glute stretching – the deep hip rotators (especially piriformis) work synergistically with the IT band, and addressing deep hip flexibility supports IT band function. Combined with IT band stretching, addressing the hip rotators produces complete lateral hip flexibility.
Side Lying Clam
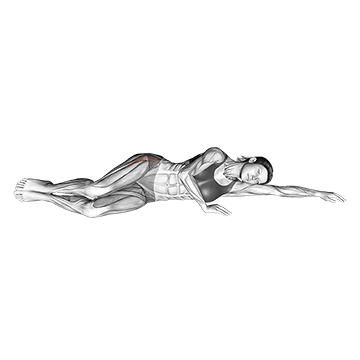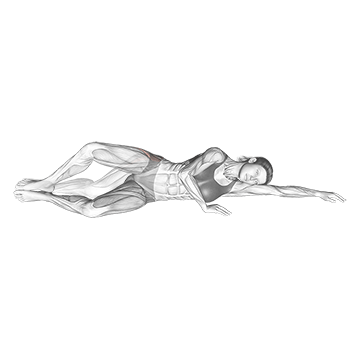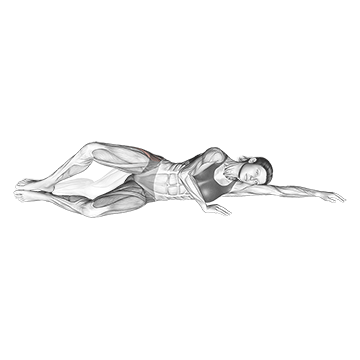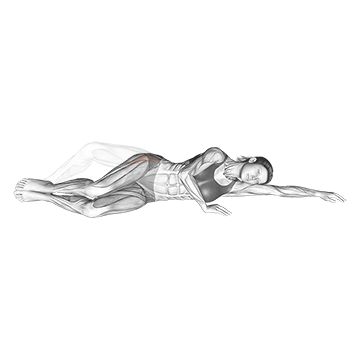
The Side Lying Clam performs clamshell exercises. The pattern produces direct gluteus medius strengthening.
For IT band syndrome correction, the clamshell produces direct gluteus medius strengthening. Run it for 3 sets of 12 to 15 reps per side, daily.
Lie on one side with knees bent at 45 degrees and stacked. Keep the feet together and lift the top knee up by externally rotating the hip. The gluteus medius works hard. Squeeze hard at peak. Lower under control. Switch sides. The pattern produces direct gluteus medius isolation – critical for IT band syndrome correction because weak gluteus medius is one of the primary contributors to IT band syndrome. The gluteus medius normally controls hip position during running and walking, and weakness produces the hip mechanics that overload the IT band. Daily clamshells address this primary cause.
Barbell Glute Bridge
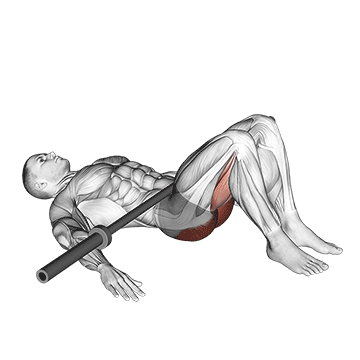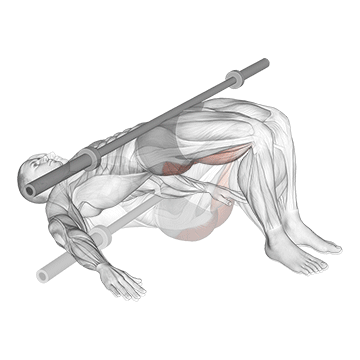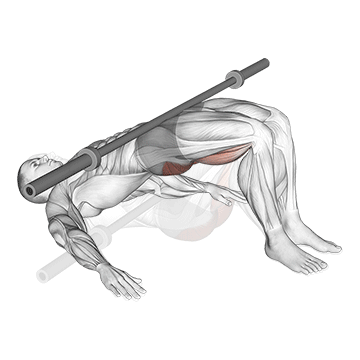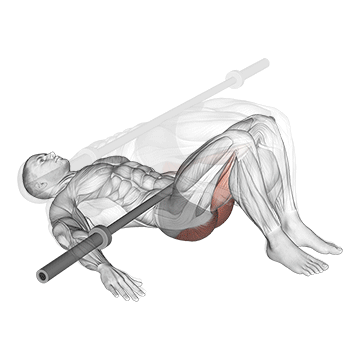
The Barbell Glute Bridge performs glute bridges. The pattern produces compound glute strengthening for IT band correction.
For IT band syndrome correction, the glute bridge strengthens glutes addressing weakness contributing to IT band issues. Run it for 3 sets of 10 to 12 reps as glute strengthening, 2 to 3 times per week.
Lie on the floor with knees bent and feet planted. Position a barbell across the hips. Drive through the heels to lift the hips up by extending the hips. The body forms a straight line from shoulders to knees at the top. The glutes work hard. Squeeze at peak hip extension. Lower under control. The pattern produces compound glute strengthening – critical for IT band syndrome correction because comprehensive glute strengthening (gluteus maximus alongside gluteus medius work) supports proper hip mechanics. Strong glutes reduce the hip stability issues underlying IT band syndrome.
Side Plank
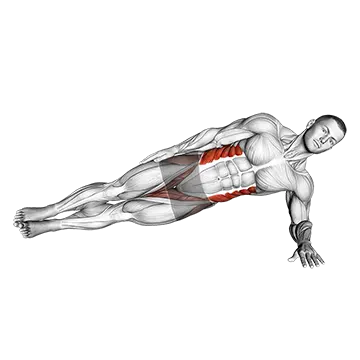
The Side Plank performs side plank holds. The pattern produces lateral core and hip stability.
For IT band syndrome correction, the side plank produces lateral core stability. Run it for 3 sets of 30 to 60-second holds per side as lateral stability work.
Lie on one side propped up on the elbow with the elbow under the shoulder. Lift the hips so the body forms a straight line from feet to head. The lateral core (obliques and quadratus lumborum) and gluteus medius work hard isometrically. Hold for the working interval. Switch sides. The pattern produces lateral core and hip stability – critical for IT band syndrome correction because the side plank trains the entire lateral chain (gluteus medius, obliques, hip stabilizers) that supports proper hip position. Excellent integrated lateral chain exercise.
Side Hip Abduction

The Side Hip Abduction performs side-lying hip abduction. The pattern produces direct gluteus medius strengthening.
For IT band syndrome correction, the side hip abduction produces direct gluteus medius loading. Run it for 3 sets of 12 to 15 reps per side, 3 to 4 times per week.
Lie on one side with the bottom leg bent for stability. Keep the top leg straight. Lift the top leg upward by abducting at the hip. The gluteus medius works hard through pure hip abduction. Lower under control. Switch sides. The pattern produces direct gluteus medius isolation through pure hip abduction – excellent for IT band syndrome correction because dedicated gluteus medius strengthening addresses the primary weakness contributing to the condition. Combined with clamshells, side hip abductions produce complete gluteus medius development.
Foam Roll Serratus Wall Slide
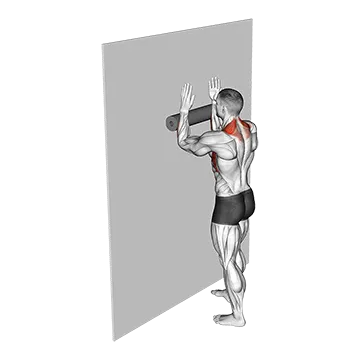
The Foam Roll Serratus Wall Slide performs foam-rolled serratus wall slides. The pattern produces upper-body postural support for integrated function.
For IT band syndrome correction, the foam roll serratus wall slide produces upper-body postural support. Run it for 3 sets of 10 to 15 reps as integrated work, daily.
Stand with a foam roller against a wall, positioned between the upper back and the wall. Press the forearms against the foam roller (or place forearms on the wall above the roller). Slide the forearms up the wall while maintaining contact between forearms and wall, with the foam roller releasing the upper back. The serratus anterior, lower traps, and posterior shoulders work hard. Lower under control. The pattern produces serratus and thoracic mobility integration – while not directly an IT band exercise, addressing thoracic and shoulder mobility supports the integrated movement chain that affects lower-body function. Daily integrated work supports overall movement quality.
Dumbbell Step Up
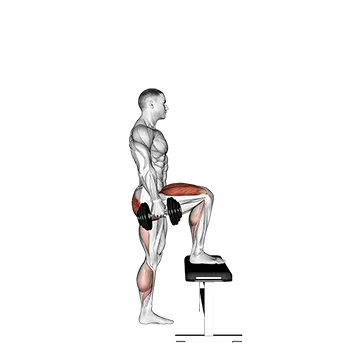
The Dumbbell Step Up performs step-ups. The pattern produces unilateral leg strengthening with hip stability.
For IT band syndrome correction, the step-up produces unilateral leg work training proper hip mechanics. Run it for 3 sets of 10 to 12 reps per leg as unilateral work, 2 times per week.
Stand in front of a bench or box about knee height holding dumbbells in each hand. Step up onto the bench with one leg. Drive through the front leg to stand fully on top of the bench while maintaining hip level (the working hip should not drop). Step back down under control. Switch legs. The pattern produces unilateral leg strengthening with active hip stability training – critical for IT band syndrome correction because step-ups train proper hip mechanics during single-leg loading, which directly translates to running and walking mechanics where IT band issues manifest. Excellent functional exercise.
Bodyweight Single Leg Deadlift
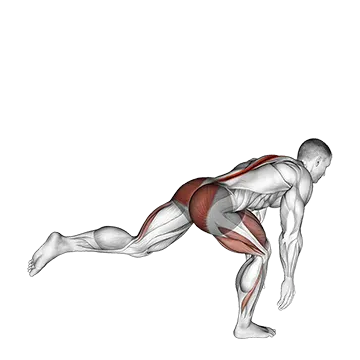
The Bodyweight Single Leg Deadlift performs single-leg deadlifts. The pattern produces unilateral hip and balance training.
For IT band syndrome correction, the single-leg deadlift produces unilateral posterior chain loading with balance demands. Run it for 3 sets of 8 to 10 reps per side, 2 to 3 times per week.
Stand on one leg with the other leg extended slightly behind. Hinge forward at the hip, lifting the back leg behind while lowering the torso forward. Keep the back flat. Reach the hands toward the floor. Drive back up to standing by extending the hip. Switch sides. The pattern produces unilateral posterior chain loading with balance and hip stability demands – excellent for IT band syndrome correction because single-leg deadlifts train integrated hip stability under load, addressing the hip mechanics issues underlying IT band syndrome.
Open Book Stretch
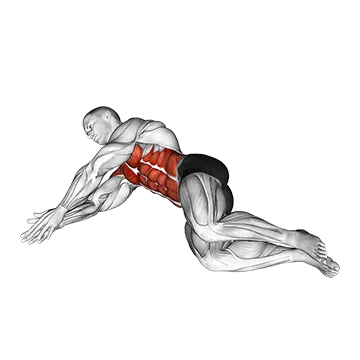
The Open Book Stretch performs thoracic mobility stretching. The pattern produces thoracic mobility supporting integrated movement.
For IT band syndrome correction, the open book stretch produces thoracic mobility supporting integrated function. Run it for 3 sets of 8 to 10 reps per side, daily.
Lie on one side with knees bent at 90 degrees and hips stacked. Extend both arms straight in front at shoulder height with palms together. Slowly rotate the top arm and torso open toward the floor behind, opening like a book. Reach the top arm to touch the floor on the opposite side. Hold briefly. Return to start. Switch sides. The pattern produces thoracic rotation mobility – supports integrated movement chain that hip function depends on. Limited thoracic mobility forces compensation patterns that can affect lower-body function.
How To Program These Workouts
A productive IT band syndrome session pulls 6 to 8 exercises from the list above. A common balanced session: standing iliotibial stretch (mobility primary – daily), seated piriformis stretch (deep hip), side-lying clam (gluteus medius primary – daily), side hip abduction (gluteus medius), barbell glute bridge (compound glute), side plank (lateral stability), dumbbell step-up (functional). For acute IT band syndrome correction phase: emphasize daily gluteus medius work (clamshells, side hip abductions) plus daily IT band stretching plus 2 to 3 weekly compound glute strengthening sessions. For maintenance phase: 3 to 4 sessions per week covering all patterns. Run gluteus medius work for 3 sets of 12 to 15 reps per side, IT band stretching for 3 sets of 30 to 60-second holds, compound glute work for 3 sets of 10 to 12 reps, lateral stability for 3 sets of 30 to 60-second holds.
Train IT band syndrome correction with daily high-frequency intervention for accelerated improvement. The condition responds best to consistent daily gluteus medius work plus regular IT band stretching plus addressing aggravating activities (typically reducing running mileage temporarily). Most successful IT band syndrome programs include: 1) daily gluteus medius work (clamshells, side hip abductions – critical for the primary weakness), 2) daily IT band stretching, 3) 2 to 3 weekly compound glute and posterior chain strengthening sessions, 4) regular cross-training (cycling, swimming) replacing some running during correction, 5) gradual return to running with proper progression, 6) addressing training errors that contributed to the issue. Most non-severe cases improve substantially within 6 to 12 weeks. Severe or persistent cases warrant medical evaluation – consider consulting a physical therapist or sports medicine professional for individualized assessment.
For broader programming, see our best workouts for runners and how to fix knee pain. For specific work, see our best gluteus medius exercises.
Final Thoughts
Fixing IT band syndrome requires applying the right intervention principles consistently over time: gluteus medius strengthening as the primary intervention (the single most important factor), IT band stretching for direct flexibility, deep glute and hip rotator stretching for the hip complex, compound glute strengthening for overall hip strength, lateral core stability, unilateral hip mechanics training, thoracic mobility, and addressing aggravating activities. The combination of IT band stretches, piriformis stretches, clamshells, glute bridges, side planks, side hip abductions, integrated mobility work, step-ups, single-leg deadlifts, and open book stretches covers every functional pattern needed for IT band syndrome correction and produces broader hip function, mobility, and athletic capacity than stretching alone. Most individuals with non-severe IT band syndrome who consistently apply these principles see measurable improvement within 6 to 12 weeks – including reduced lateral knee pain, improved tolerance for running and cycling, addressed gluteus medius weakness, better hip mechanics during single-leg activities, and the integrated lower-body function that supports overall athletic performance. For most non-severe IT band syndrome cases, dedicated exercise-based correction is one of the most effective interventions available.
Stay focused on gluteus medius strengthening as the absolute priority for IT band syndrome correction. The most common mistake people make is doing only IT band stretching or foam rolling without addressing the gluteus medius weakness underlying the condition. The fix: prioritize daily clamshells and side hip abductions (the two most direct gluteus medius exercises) as the foundation of correction work. Combined with IT band stretching, compound glute work, lateral stability training, and addressing training errors, dedicated gluteus medius work produces the IT band syndrome correction that stretching-only or foam-rolling-only approaches never achieve. IT band syndrome correction depends primarily on addressing the gluteus medius weakness underlying the condition – this is the central insight in modern IT band syndrome management.
Frequently Asked Questions
How do I fix IT band syndrome?
Daily gluteus medius work plus IT band stretching plus reduced aggravating activities. Daily clamshells and side hip abductions (3 sets of 12 to 15 reps each, daily) address the primary cause – gluteus medius weakness. Daily IT band stretching addresses the flexibility component. Combined with glute bridges (compound glute), side planks (lateral stability), step-ups (functional hip mechanics), single-leg deadlifts (unilateral hip stability), and reduced running mileage temporarily, this comprehensive approach produces measurable improvement. Most non-severe cases see improvement within 6 to 12 weeks. Severe or persistent cases warrant evaluation by a healthcare provider.
What causes IT band syndrome?
Weak gluteus medius is the primary cause. Most IT band syndrome develops from: 1) weak gluteus medius – the primary contributor producing hip mechanics that overload the IT band, 2) tight IT band and lateral hip muscles, 3) weak gluteal complex, 4) training errors (rapid mileage increases, overtraining), 5) limited hip mobility, 6) muscle imbalances, 7) inadequate cross-training, 8) cumulative effect of multiple factors. Most cases involve multiple factors but gluteus medius weakness is consistently the central issue. The fix combines gluteus medius strengthening, IT band stretching, and addressing training errors.
How long does IT band syndrome take to heal?
6 to 12 weeks for measurable improvement in most non-severe cases. Most people who consistently apply daily gluteus medius work plus IT band stretching plus addressing training errors see measurable improvement within 6 to 12 weeks. Beginners often see initial gains within 4 to 6 weeks. Severe cases may take 12 to 16+ weeks. Persistent cases (those not improving after 12 weeks of consistent treatment) warrant medical evaluation. Cases with severe pain warrant immediate medical evaluation. Daily consistency matters more than session intensity for sustainable IT band syndrome resolution.
What’s the best exercise for IT band syndrome?
Daily clamshells plus side hip abductions plus IT band stretching. Clamshells produce the most direct gluteus medius loading possible – the single most important exercise for IT band syndrome. Side hip abductions provide additional direct gluteus medius isolation. Combined with standing IT band stretches, piriformis stretches (deep hip), glute bridges (compound glute), side planks (lateral stability), step-ups (functional), single-leg deadlifts (unilateral hip), and integrated mobility work, clamshells plus side hip abductions plus IT band stretches form the foundation of IT band syndrome correction.
Should I keep running with IT band syndrome?
Reduce running temporarily and consult a healthcare provider for severe or persistent symptoms. Most successful IT band syndrome correction involves temporarily reducing running mileage during the acute phase, replacing some running with cross-training (cycling, swimming, strength training), focusing on gluteus medius strengthening, and gradually returning to running as symptoms improve. Continuing to run through significant pain can worsen the condition. The combination of reduced running plus dedicated correction work produces faster recovery than continued running. Consider consulting a physical therapist or sports medicine professional for individualized return-to-running progression.







